Mephedrone (4-methylmethcathinone) is a synthetic cathinone, a class of psychoactive substances derived from the khat plant (Catha edulis). Mephedrone has been associated with numerous cases of overdose, resulting in severe health complications and fatalities. Overdose cases have been reported, leading to severe health complications and fatalities. This article aims to provide a comprehensive review of mephedrone overdose and the necessary pre-hospital care required for effective management.
Risk factors for mephedrone overdose
Several risk factors can contribute to the possibility of mephedrone overdose. First aid in a mephedrone overdose
-
First, combining mephedrone with other psychoactive substances (including alcohol) can multiply the likelihood of overdose symptoms, and there is no way to medically prevent these factors. Stimulants have many cardiovascular effects, including increased heart rate and blood pressure, sometimes to dangerous levels. If a person uses different types of stimulants at the same time, it can put them at additional risk for catastrophic cardiovascular events, including heart attack and stroke, as well as other potentially serious health consequences associated with overdose.
-
Second, the presence of co-occurring psychiatric disorders, past emotional trauma, and pathologies for which antipsychotics or antidepressants are taken can also cause undesirable consequences. For example, if a person has schizophrenia or bipolar disorder, using mephedrone can lead to unforeseen conditions associated with exacerbation of pathologies, as well as uncontrolled use of mephedrone and injuring oneself or others. Also, if a person is using a certain class of antidepressants, it can lead to the development of serotonin syndrome.
-
Finally, physical activity is an important risk factor. When a person is in a room where it is stuffy, or if the person is actively moving (dancing, physical activity, and so on), this increases the risk of unwanted side effects many times over.
-
The use of mephedrone, theoretically, does not contribute to the development of a metabolic disorder. However, it increases the severity of diabetes symptoms, disrupts the control and compensation systems of regulating the glycemic profile, decreases the effect of pharmacological therapy of diabetes mellitus. Therefore, the use of mephedrone is not recommended for patients with diabetes mellitus.
Clinical Manifestations of Mephedrone Overdose (Symptoms of mephedrone overdose)
Typically, mephedrone overdose occurs in long term sessions due to an increase in each subsequent dose, or in “mephedrone marathons”. Sometimes an overdose occurs with a single use when the dose is too high for the body.
Mephedrone overdose can present with a wide range of symptoms, including:
- Cardiovascular: tachycardia, hypertension, chest pain, and palpitations;
- Neurological: agitation, confusion, seizures, and coma;
- Psychiatric: anxiety, paranoia, hallucinations, and suicidal ideation;
- Gastrointestinal: nausea, vomiting, and abdominal pain;
- Respiratory: tachypnea, dyspnea, and respiratory failure.
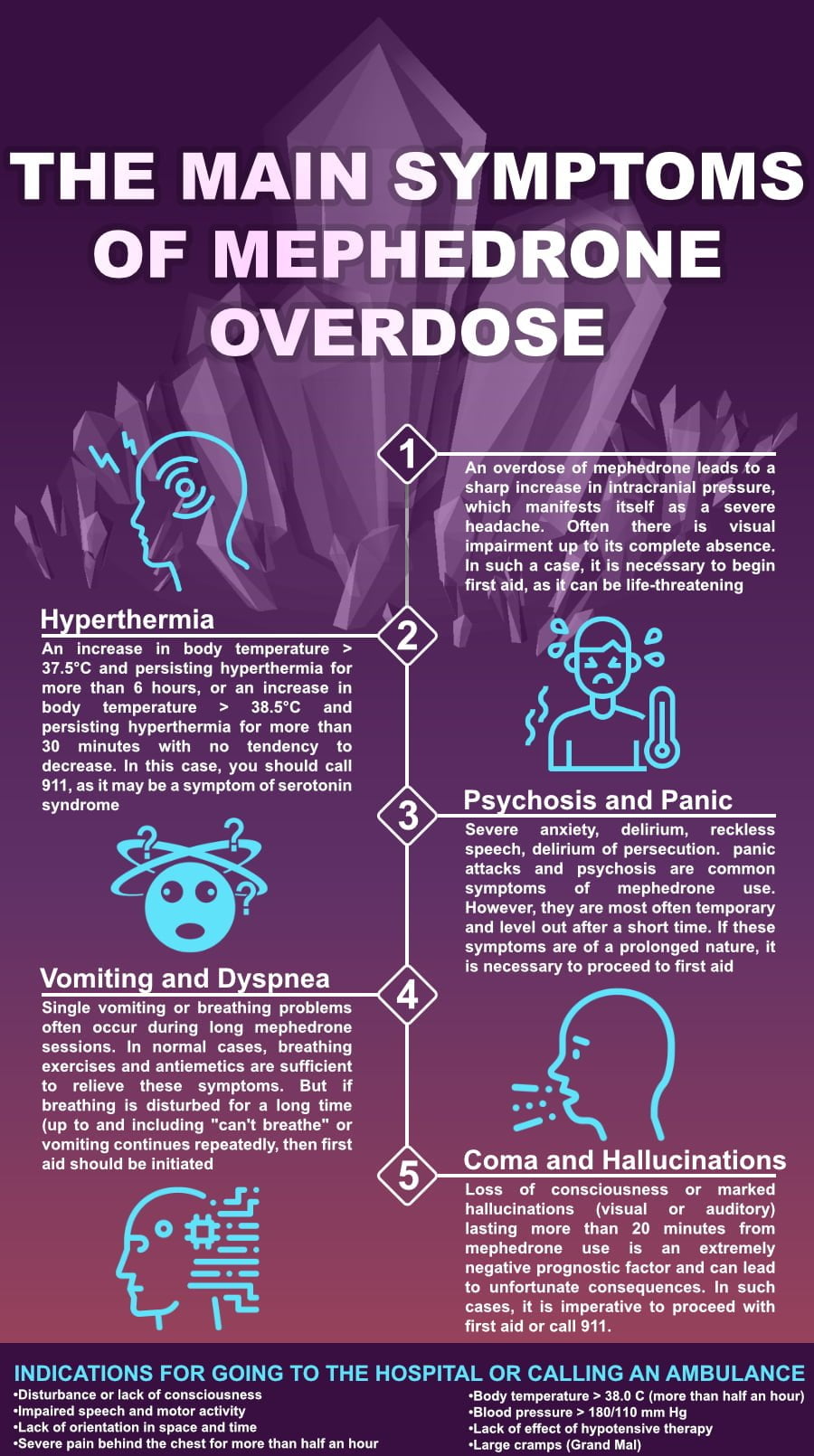
The following are the main symptoms of mephedrone overdose:
- Loss of consciousness.
- Repeated vomiting.
- Severe non-localized or localized pain in the head.
- Sharp impairment of vision up to its absence and lasting more than 10 minutes.
- Expressed anxiety, psychosis, panic attack.
- Delirium, reckless speech, delirium of persecution.
- Disturbance of breathing up to and including “inability to breathe.”
- Hallucinations or visual and auditory illusions lasting more than 20 minutes from the time of mephedrone use.
- An increase in body temperature of more than 37.5C and persisting hyperthermia for more than 6 hours, or an increase in body temperature of more than 38.5C and persisting hyperthermia for more than 30 minutes with no tendency to decrease.
First aid in a mephedrone
Indications for going to the hospital or calling an ambulance:
-
Disturbance or lack of consciousness
-
Impaired speech and motor activity
-
Lack of orientation in space and time Severe pain behind the chest for more than half an hour
-
Body temperature over 38.0 C and persistence of hyperthermia for more than half an hour
-
Blood pressure over 180/110 mmHg or no effect of conservative hypotensive therapy
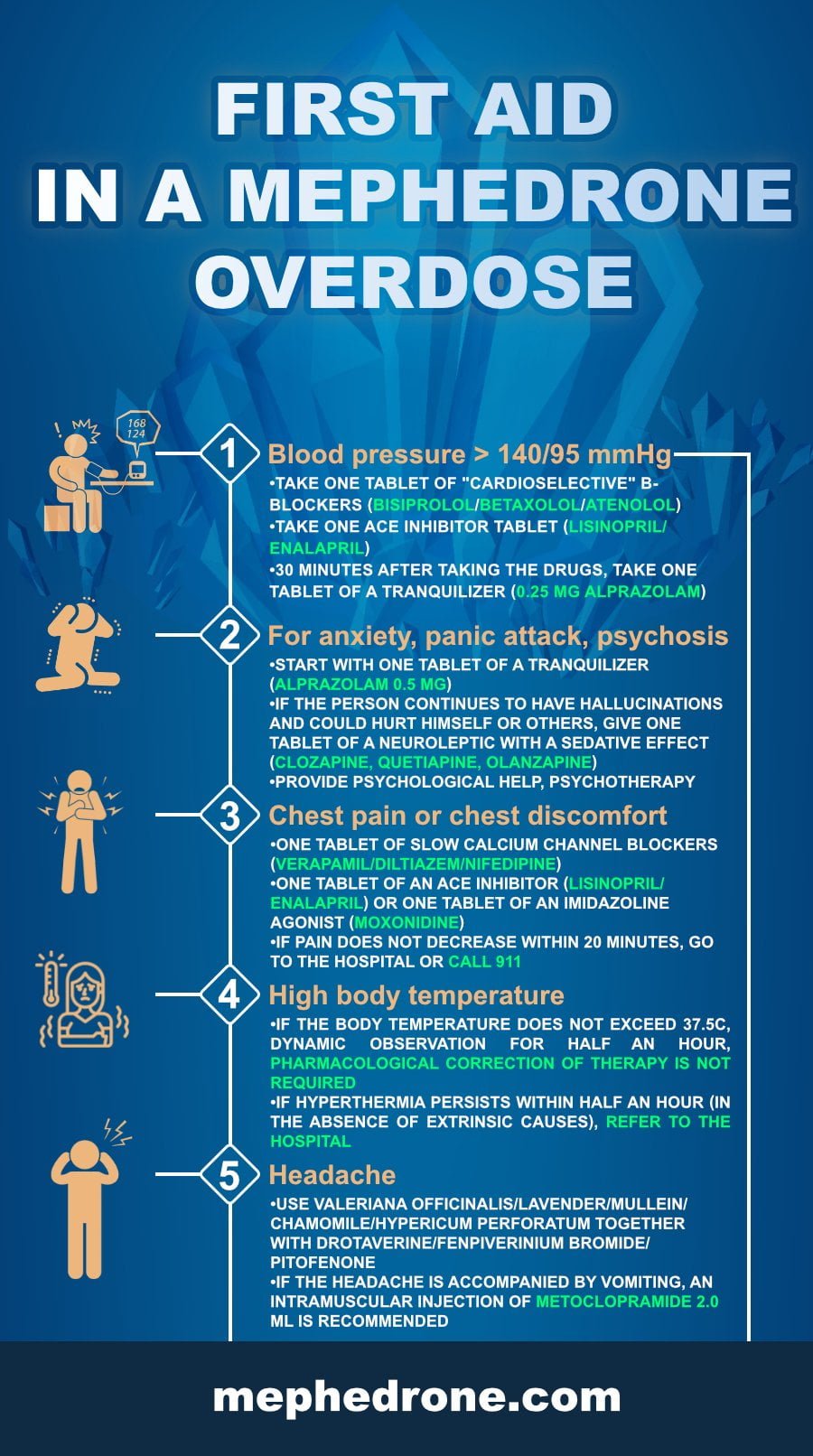
If blood pressure rises above 140/95 mmHg
-
Take one tablet of “cardioselective” β-blockers (bisiprolol/betaxolol/esmolol/atenolol)
-
Take one ACE inhibitor tablet (lisinopril/enalapril)
-
30 minutes after taking the drugs, take one tablet of a tranquilizer (0.25 mg alprazolam).
For anxiety, panic attack, psychosis
-
Start with one tablet of a tranquilizer (alprazolam 0.5 mg)
-
If the person continues to have hallucinations and could hurt himself or others, give one tablet of a neuroleptic with a sedative effect (clozapine, quetiapine, olanzapine)
-
Provide psychological help, psychotherapy for emergencies.
Chest pain or chest discomfort
-
One tablet of slow calcium channel blockers (verapamil/diltiazem/nifedipine, which reflexively reduce heart rate
-
One tablet of an ACE inhibitor (lisinopril/enalapril) OR one tablet of an imidazoline agonist (moxonidine)
-
If pain does not decrease within 20 minutes, go to the hospital or call 911.
High body temperature
-
If the body temperature does not exceed 37.5C, dynamic observation for half an hour, pharmacological correction of therapy is not required
-
If hyperthermia persists within half an hour (in the absence of extrinsic causes), refer to the hospital.
Headache
For headaches, the use of antispasmodic drugs in combination with herbal sedatives or tranquilizers in low doses is recommended. For example, use valeriana officinalis/lavender/mullein/chamomile/hypericum perforatum together with drotaverine/fenpiverinium bromide/pitofenone. If the headache is accompanied by vomiting, an intramuscular injection of metoclopramide 2.0 ml is recommended (or use the tablet form in a dose of 40 mg). In isolated nausea and functional dyspepsia, pharmacological therapy is not required.
Cramps
Tranquilizers are recommended for tremors, small or urinary seizures, or mild psychomotor agitation, but not neuroleptics!
Grand-mal seizures can be divided into different types depending on their origin, symptoms, and severity. Understanding the different types of grand mal seizures and their severity can help you recognize a seizure and respond appropriately. Listed below are the most common types of seizures:
-
Generalized Seizures: generalized seizures affect both sides of the brain and often involve loss of consciousness. There are several subtypes of generalized seizures, including:
-
Tonic-Clonic Seizures: these seizures are characterized by stiffening of the body (tonic phase) followed by jerking movements (clonic phase) and loss of consciousness. they are the most common type of seizure and can be very dangerous.
-
Absence Seizures: these seizures cause brief episodes of staring or loss of awareness, often mistaken for daydreaming.
-
Myoclonic Seizures: these seizures involve sudden, brief muscle jerks that can affect different parts of the body.
-
Atonic Seizures: these seizures cause sudden loss of muscle tone and can cause falls or head injuries.
-
Focal Seizures: focal seizures originate from a specific area of the brain and can cause a wide range of symptoms, depending on the location of the affected area.
So, if you witness a seizure, here are steps you can take to provide first aid:
-
Stay calm – Stay calm and keep the person safe. Try not to let them fall or hit their head on a hard surface. Remove any objects that could cause harm, such as sharp objects, glasses, or furniture.
-
Seizure time – note the time the seizure started and how long it lasted. This information may help health care providers diagnose and treat the person. Contact emergency services if it lasts more than five minutes.
-
Protect the victim’s head – gently place something soft, such as a pillow, sweater, or jacket, under the victim’s head.
-
Loosen tight clothing – loosen tight clothing around the person’s neck or waist to make it easier for them to breathe.
-
Roll the person onto his side – slowly and carefully roll the person onto his side so he does not choke on vomit or saliva. When seizures stop, a recovery position may be appropriate.
-
Stay with the person – stay with the person until they are fully recovered or until medical emergencies arrive. Calm them down and talk to them calmly.
Conclusion
In conclusion, mephedrone overdose is a serious public health and drug-using society issue that requires prompt recognition and appropriate first aid intervention. As the prevalence of mephedrone use continues to rise, it is critical that the public is well informed about the signs and symptoms of mephedrone overdose, as well as the necessary first aid steps to be taken in such situations.
Education and awareness campaigns should be implemented to disseminate accurate information about the risks associated with mephedrone use and the importance of seeking immediate medical assistance in case of an overdose. Furthermore, harm reduction strategies, such as providing access to drug testing services and promoting responsible drug use, can help minimize the occurrence of mephedrone overdoses.
In the event of a mephedrone overdose, the primary goals of first aid are to keep the person safe, stabilize their condition, and facilitate access to professional medical care if needed. Basic first aid measures include assessing the person’s level of consciousness, monitoring vital signs in case of impaired consciousness, providing supportive care and contacting emergency medical services if necessary.
As we continue to advance our knowledge of mephedrone and its effects on the human body, it is our hope that this publication will serve as a valuable resource for those seeking to provide life-saving first aid in the face of a mephedrone overdose. By equipping ourselves with the necessary skills and knowledge, we can make a meaningful difference in the lives of those affected by this dangerous substance and contribute to the ongoing efforts to combat the global drug crisis.